Woman's Health
Imbalance of the Vaginal Flora
A woman's vaginal flora is an important protective shield against harmful germs. Billions of different lactobacilli - also called lactic acid bacteria - ensure an acidic pH value (3.8-4.5) in the vagina in which pathogenic bacteria and fungi cannot multiply. This protection is particularly important to keep all of women's reproductive organs healthy and functioning.
The development of the vaginal flora starts right from birth through the oral intake of good bacteria. These symbionts know exactly their destination in the human body, and they are able to find their place within a very short time. It is therefore essential, especially after taking antibiotics, but also when other problems in the vaginal area occur, to reintroduce exactly those bacteria orally, which then colonise the vagina in a short amount of time.

Symptoms and Treatment
Bacterial Vaginosis
Bacterial vaginosis is often associated with a yellowish-greenish and unpleasant fishy-smelling discharge. Sexual intercourse may occasionally cause pain. The most important sign is the imbalance of the vaginal flora - the pH value is over 4.5. In addition to itching, you may experience pain in the vaginal area and lower abdomen, as well as discomfort during sexual intercourse. BV is primarily treated with oral or topical antibiotics (metronidazole, clindamycin). However, this treatment is not recommended for use during the first trimester of pregnancy. Due to the increased risk of BV, especially during pregnancy, the question arises of what alternative we have to treat the condition.
Usually, a polymicrobial biofilm adheres to the vaginal epithelium in the presence of BV - typical of chronic infections. This biofilm is not removed with any treatments used to date, which is why BV very often occurs with chronic recurrence. After 3 months, only 60-70% of those affected are free of symptoms, after six months the healing rate is far lower.
According to the latest findings, supplementing certain Lactobacillus strains gives us the possibility to significantly reduce the recurrence of BV after previous treatment with antibiotics or azides to lower the vaginal pH value. The use of probiotics can reduce the BV recurrence rate by about half (AWMF, 07/2013). A contemporary form of taking probiotics containing numerous Lactobacillus strains is by drinking a mixed probiotic formula. This is actually the natural way in which probiotic bacteria colonise the vaginal tract from the birth onwards. Studies show that the rectum/gut plays an important role as a reservoir for lactobacilli that colonise the vaginal tract (Petricevic, 2012). Orally taking a probiotic can avoid additional irritation of the already irritated vaginal mucosa caused by chemical additives in capsule shells and suppositories, and the natural moistening of the vagina takes place within a few days through the metabolic products of lactobacilli.
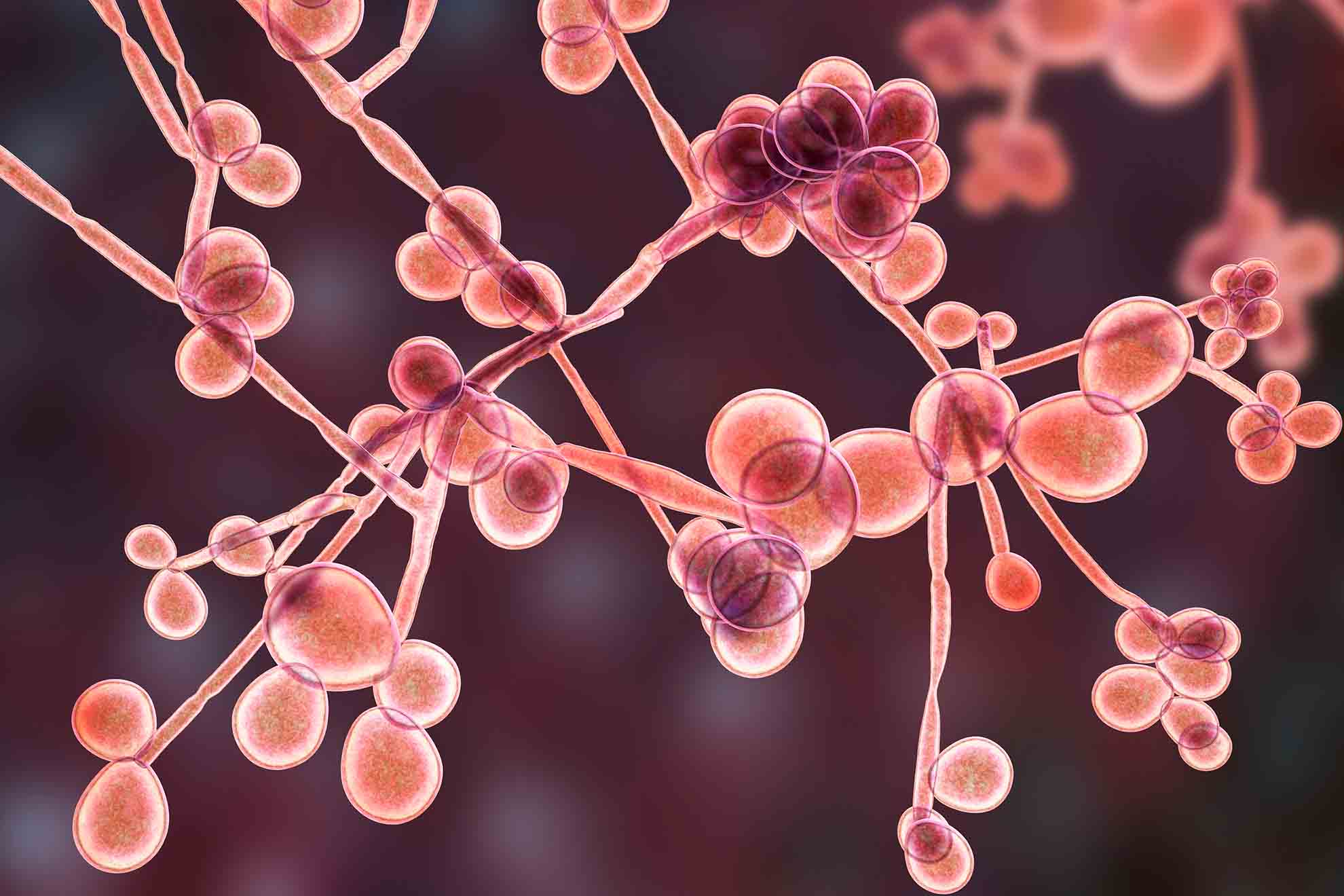
Candida albicans
Symptoms and Treatment
Vaginal Thrush
Vulvovaginal candidiasis (VC), also known as vaginal thrush, is also one of the most common infections of the female genital tract. Between 70 and 75% of women are affected at least once in their lives, and up to 50% of women experience frequent recurring infections. The most common cause of this yeast fungus is Candida albicans (in 85-90% of cases).
The most common symptom of vaginal thrush is itching, and there is also a change in discharge (thin to flaky), vaginal redness, soreness, burning, pain during sexual intercourse and when urinating.
Thrush is usually treated with local or oral antimycotics, although there are also restrictions on use during pregnancy. In addition, Candida glabrata is not sufficiently sensitive to the usual dosages of all antimycotics approved for gynecological purposes (AWMF, 12/2013). This is precisely why the importance of probiotics is increasing. Lactobacillus strains have already been identified that significantly reduce vaginal colonisation with pathogens and they can also play a protective role in VC.
"A healthy vaginal flora consists mainly of different types of lactobacilli, which play a central role in protecting the urogenital tract from pathogens and infections through their production of lactic acid."
A mother passes on the intestinal bacteria to her baby
The colonisation of the human organism with microorganisms largely determines the lifelong resistance of our immune system. “Here, both the birth and probably the pregnancy itself are crucial. During birth, the newborns come into contact with the mother's bacterial flora and therefore can build up their own immune system,” explains Prof. Huber. The decisive factor here is that the mother has a healthy, balanced bacterial flora, especially in the intestine. "In the gut?" you may ask. That's right! The intestine is the reservoir for colonisation of the vagina; if the intestinal flora is healthy and rich in important lactobacilli, then the same applies to the vaginal flora. Through the passage of the birth canal, the child comes into close contact with the mother's bacterial flora. This forms the basis for colonisation of the child's intestines and the basis for the development of the child's immune system.
However, a newborn only benefits from this during a vaginal birth - and not during a caesarean section. C-section delivery is, however, on the increase, especially since the babies in the mother's wombs are growing larger (head and shoulder circumference) and the female pelvis cannot keep up with this evolutionary spurt. Prof. Huber: "At the moment, a big topic in gynecology is how to support newborns with the mother's intestinal and vaginal bacteria postpartum, even after a caesarean section."

Gut Bacteria and Hormones
Intestinal bacteria and their interaction with the hormone balance is becoming an area of increased focus. Initial research results indicate that the intestinal microbiome plays a central role in regulating endogenous hormones and could therefore influence the risk of developing hormone-related diseases.